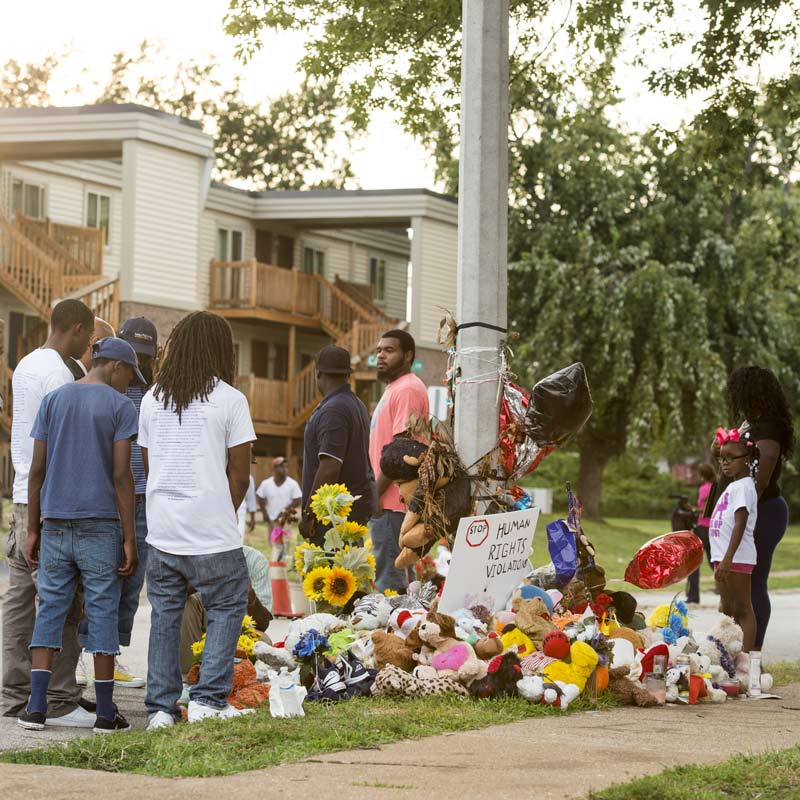Two years ago today, the shooting death of Michael Brown astounded a nation, and forever changed the way that we talk about race and health in America. The Ferguson Commission’s report, which was released last September, suggested that health disparities were a key factor in the unrest that began after Brown’s death. The report suggests that preparing public school teachers with basic mental health skills, establishing more trauma support, and expanding Medicaid in Missouri – among other things – would help eliminate some of the issues that were plaguing Ferguson and the St. Louis region.
The Commission’s findings, grounded in an inclusive, community-wide process, identified the social and economic factors that shaped the circumstances of Michael Brown’s death and the events that followed. Racism, lack of economic opportunity, discrimination, and poor access to basic goods and services – healthy food, transportation, schools, affordable housing, and safe neighborhoods – all contributed. The Ferguson neighborhood where Michael Brown lived and died reflected these challenges, as do numerous neighborhoods across the St. Louis region and the country.
The social and economic factors documented in the Ferguson Commission’s report have also resulted in stark differences in the health of black and white Americans. Extensive research over the past several decades shows that blacks receive poorer care in our health care system and have a disproportionately difficult time getting access to care in the first place. As a result of social and economic factors, blacks get sick sooner, have more severe symptoms when they do get sick, and die at younger ages. For all of the appropriate recent attention given to the increase in middle-aged whites’ mortality rates, there was little attention to the fact that, even with that increase, black mortality rates remain 40 percent higher than white mortality rates. And Missouri’s mortality rates for both blacks and whites are higher than the national average.
Black-white health differences are evident in the quality of care received within the health care system; in access to preventive and specialty care; and in life opportunities, exposures, and stresses that influence underlying health status. Racism and discrimination are two stress factors shown to have negative impacts on health, causing an increase in depression, cardiovascular disease, breast cancer, and mortality. And black people who experience frequent racism are more susceptible to heart disease, hypertension, diabetes, and stroke.
Michael Brown’s death came after Trayvon Martin’s, and the events following Brown’s death were communicated widely and in real time via social media. These circumstances resulted in widespread recognition of a pattern of violence, affecting us all, which has been reinforced over the past two years by one tragedy after another. The factors underlying this pattern of violence also lead to worse health outcomes for blacks. The commemoration of Michael Brown’s death serves as a reminder to us – in St. Louis and across the country – that we have significant work to do to make fundamental progress on these issues if we want to succeed in becoming healthier and more economically equitable in the future. All of us deserve the opportunity to lead healthy lives in healthy communities.