Pre-existing conditions, a term of art in the health insurance industry, has garnered widespread attention recently. What began in the 1930s as a list of diseases or conditions used to not enroll people most likely to use health insurance became a staple of profitable health insurance businesses. The industry benefits financially from enrolling healthier people, not the people who will actually need care. The idea of systematically excluding people from health insurance via pre-existing conditions raises the question: On what basis should we keep people from being covered?
Pre-existing conditions, a term of art in the health insurance industry, has garnered widespread attention recently. What began in the 1930s as a list of diseases or conditions used to not enroll people most likely to use health insurance became a staple of profitable health insurance businesses. The industry benefits financially from enrolling healthier people, not the people who will actually need care. The idea of systematically excluding people from health insurance via pre-existing conditions raises the question: On what basis should we keep people from being covered?
Health insurance has roots in two competing values: mutual benefit and profitability. One origin of health insurance was the shared obligation among members of professional groups, such as teachers. These obligations were embodied in nonprofits like Blue Cross that were regulated by states as community benefits. The other origin was the business model, which incentivizes the exclusion of people with medical conditions that are predicted to be high utilizers of care. Pre-existing conditions typically are defined medically (e.g., diabetes, coronary artery disease, AIDS/HIV, and alcohol abuse). Over 1 million Missourians under 65 have such pre-existing conditions, 30 percent higher than the national average. Under the Affordable Care Act there are now regulations, supported by widespread public consensus, that put strong limits on health insurance plans’ use of pre-existing conditions to reject people.
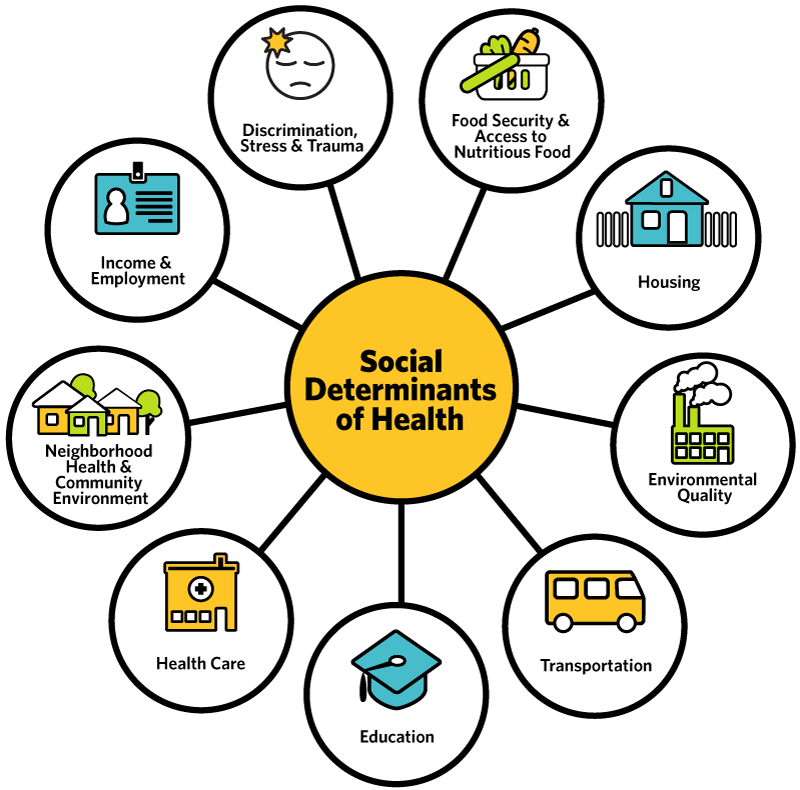
But as medicine expands its understanding of the institutional determinants of health, pre-existing conditions can be viewed more broadly, as structural forces to be addressed in clinical practice. Often lumped under the phrase “social determinants of health,” these structural factors have more influence on people’s health than medical care. So, it is reasonable to find out if these factors also influence the ability to get health insurance and ask: What are the social and systemic pre-existing conditions that we use to determine who has health insurance and who does not? Recent experience in Missouri suggests poverty is one of the most important of these.
Missouri’s Medicaid program provides health insurance for close to a million low-income Missourians. Last year saw a drop of 77,000 enrollees, more than 7 percent, and most of these were children and women of child-bearing age. The primary cause of this precipitous drop was technological and administrative changes in the enrollment and verification systems, not changes in the actual eligibility status of those dropped from enrollment.
For those of you with employer-based insurance, imagine for a moment how you and your colleagues would be affected if your insurance coverage ended because of administrative changes initiated by your insurance company. When health insurance stops abruptly and unexpectedly, it disrupts people’s lives. Sudden loss of insurance stops access to prescription drugs and primary care, which in turn can affect adults’ ability to work or children’s school attendance. The recent decline in Missouri’s Medicaid coverage demonstrates that it is mainly changes in institutional practices of Medicaid, not the behavior of enrolled children or families, that triggered 77,000 Missourians to lose coverage. For these people, having a low income is a pre-existing condition.
The health effects of living in poverty was underscored at the 2019 Poverty Summit I recently attended in Branson, Missouri, hosted by the College of the Ozarks. Poverty is one of the strongest predictors of poor health, and poor health contributes to poverty. Speakers at the summit, including local leaders from education, philanthropy, and nonprofits helping poor residents of Stone and Taney Counties, described families’ need for food, housing, transportation, social services, employment, education, and health care. A constant challenge for families, highlighted by many speakers, is that people living in poverty don’t experience these needs individually. Daily they’re forced to make trade-offs between food or rent, electricity or a clinic visit, and if that clinic visit ends with a written prescription, between getting it filled or buying a bus ticket to get to work. Poverty means being unable to meet your basic human needs and choosing which ones to do without, including health care. These trade-offs show that losing Medicaid coverage leads to poor health not only by limiting health care, but it also forces choices that put greater strain on the entire safety net. Recent research on Medicaid confirms this; Medicaid not only helps with health care, it addresses financial insecurity – Medicaid coverage was associated with a decline in evictions, bankruptcies, and wage garnishments. Put simply, Medicaid is a hugely important component of #TheNetBenefit for all Missourians.
Most families in poverty defer seeking health care as long as possible to avoid the costs, until pain or illness demands an emergency room visit, with the ER becoming a de facto health care safety net. Across Missouri more and more families are facing trade-offs as affordability becomes an issue for people who are under-insured, losing coverage, or experiencing ever-increasing out-of-pocket payments. As more Missouri families are forced to choose between health care and other basic needs, finding a way to provide affordable care for everyone becomes more compelling. That, of course, means poverty would no longer be a pre-existing condition.